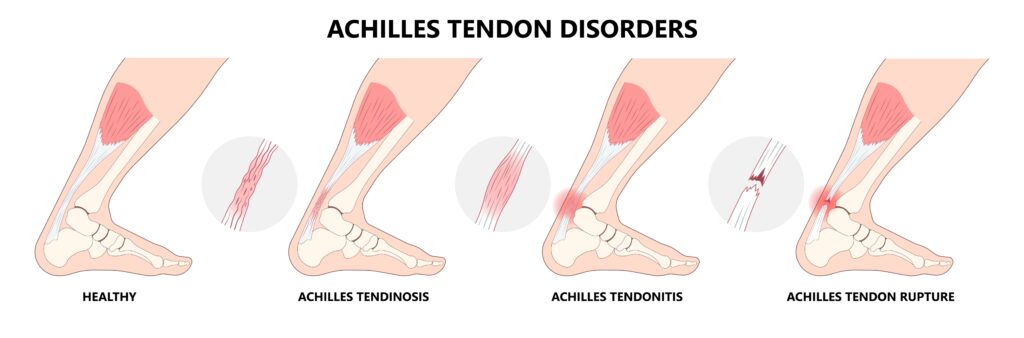
Achilles Tendonitis (Tendonosis)
The Achilles tendon is the tendon of the gastrocnemius and soleus muscles of the posterior leg and connects these muscles to the heel bone (calcaneus). It is located along the lower back portion of the calf and runs to the heel. This muscle tendon group is responsible for plantar flexion of the ankle and is the primary motor for standing and walking on the toes and powers push off when a person runs or jumps.
Injury usually results when the tendon is stressed by short quick movements or sudden starts and stops such as in Racquetball, tennis, football, or dance. It can also affect women who frequently wear high-heeled shoes and switch to sneakers to exercise. This stress could be cumulative or develop from a single spontaneous movement following an insufficient “warm-up” or stretch.
Inflammation of this tendon is known as Achilles Tendonitis. It is a degenerative condition of the tendon either in its substance or at its insertion point on the heel. Although is it commonly called tendonitis, there is no evidence of true inflammation. Achilles Tendonosis is probably a more medically correct term. It occurs when the overstressed tendon becomes degenerate causing enlargement of the tendon, restricted flexibility and pain.
Typically this condition occurs in patients with IGC (Idiopathic gastrocnemius contracture). In this extremely common condition, which predisposes to at least one half of all common foot and ankle disorders, the gastrocnemius muscle/tendon unit is excessively tight. It is diagnosed on the clinical basis in the clinic by doing the Silfverskiold test.
The important point of anatomy is that the gastrocnemius muscle originates above the knee and is tighter when the knee is extended than when it’s flexed. If the ankle can be placed into more dorsiflexion (toes pointing towards the nose) when the knee is bent than when the knee is extended, then the gastrocnemius muscle is contracted. To qualify as normal, a person needs at least 10 degrees of ankle dorsiflexion with the knee extended. Many authorities believe that the actual normal measurement should be 18 degrees. Unquestionably, less than 10 degrees is abnormal and predisposes patients to Achilles Tendonosis and other tendon disorders, plantar fasciitis, ankle sprains, bunions, and most other disorders of the forefoot!
If Achilles Tendonosis is untreated, it could grow progressively worse and a small tear may lead to tendon rupture, separating the calf muscle from the heel bone. When this occurs, normal movement of the ankle is impossible.
If Achilles Tendonosis is treated before tendon rupture, there are a number of non-operative ways to recover strength to the area. They include stretching, ice, shoe modifications, nutritional supplements, and alterations in an individual’s training schedule. The most important treatments are stretching and lengthening contraction of the gastro soleus muscle complex. Still, the best treatment is prevention. Tendonitis can be avoided with the proper strengthening of all muscle groups in the leg, along with adequate stretching and warm-ups before and after demanding activities or sports.
In certain patients, these measures are unsuccessful. Most recently, platelet rich plasma injections have become popular, but they have now been proven to be no better than a placebo. Other surgical measures have had only spotty success. Release of the gastrocnemius tendon, while leaving the soleus muscle-tendon unit untouched is known as the Strayer procedure. It is a highly simple and inexpensive procedure done in the Day Surgery section of the hospital, and followed for a short period of immobilization and then exercises. It will consistently improve the dorsiflexion of the ankle, and remove the excessive tension off the Achilles tendon allowing it to heal on its own.
Achilles Tendon Rupture
A complete rupture often occurs spontaneously during sports, without pre-existing tendonitis, usually in the athlete in his/her 30s or 40s. Most patients will say that they heard a loud pop, and it felt like their calf was going to explode. Swelling is considerable and it is difficult to walk. Historically, those athletes would elect to undergo surgical treatment to repair the tendon, followed by a period of cast immobilization. The rational to do surgery was that there would be better ultimate strength and a lower incidence of rerupture. The downside of surgery was complications usually associated with poor wound healing. Nonsurgical treatment was historically reported to carry a higher incidence of rerupture, but of course no wound healing issues.
In the past couple of years, accelerated rehabilitation of both the operated and unoperated case has narrowed the gap between the two groups. At this point in time, the rerupture rate and the ultimate strength is nearly the same for operated and unoperated cases. Surgical complications can still occur in the operated cases, but on average those patients return to work about three weeks earlier than the unoperated patients. Operated patients are back in sports by three months, the unoperated patients are back in about six months. Dr. Sanders has extensive experience in both treatment plans and since they lead to similar results, he leaves the decision with the patient.
